AUCTORES
Globalize your Research
Case Report
*Corresponding Author: I and II Degree Specialist in Comprehensive General Medicine, Faculty of Medical Sciences of Sagua la Grande. Villa Clara. Cuba.
Citation: Lázaro Martín M.E, Lázaro M. Aparicio, Leonardo M. Aparicio, Roberto M.C, Eduardo M. Cairo, et all., (2024), Axillary Artery Injury Case Report and Discussion, J. General Medicine and Clinical Practice, 7(17); DOI:10.31579/2639-4162/229
Copyright: © 2024, Claribel Plain Pazos. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Received: 01 October 2024 | Accepted: 09 October 2024 | Published: 17 October 2024
Keywords: oral submucous fibrosis; antifibrotic therapy; regenerative medicine; bioactive materials; platelet-rich plasma; laser surgery; tissue healing
The management of vascular trauma constitutes a great challenge for trauma surgeons; axillary artery injuries have a high mortality rate and are rare, so most surgeons have very limited experience in their treatment. Objective: Present a clinical case and discuss the management of axillary artery trauma and review the literature. A patient with a stab wound to the left shoulder was presented, surgical treatment, literature review and case analysis were performed.
Stab injuries are frequent injuries to the limbs, especially in the upper limb, they represent 30% of all vascular traumas, the main etiology being penetrating trauma, it is an emergency situation that we can face in the unit. emergency, it can cause the death of the patient if timely management is not carried out [1, 3].
Peripheral vascular trauma is defined as injuries to blood vessels (arterial and venous); 3% of all injuries in trauma have a vascular component, establishing a major public health problem given its lethality and complications [4].
The causes of vascular trauma can be very diverse and the types of injuries will depend on the mechanism that caused them. Hemorrhage is the first manifestation of vascular trauma, being identifiable mainly by bleeding, or sometimes being contained, evolving as a hematoma [5].
The management of vascular trauma constitutes a great challenge for trauma surgeons; axillary artery injuries have a high mortality rate and are rare, so most surgeons have very limited experience in their treatment. The axilla is a complex anatomical region due to the interrelationship of the neurovascular package at this level [6].
Definitive control of vascular injury represents a surgical challenge, especially in patients with hemodynamic instability. A patient is presented with a penetrating stab wound on the anterior aspect of the left shoulder, with injury to the axillary artery, we reviewed the topic.
A 30-year-old white male patient is brought to the emergency department with active bleeding, caused by a stab wound. He is urgently examined and has an open injury on the lower anterior aspect of the left shoulder, about two centimeters long, with significant bleeding. First aid is provided and he is taken to the room to control the bleeding. The emergency team made up of vascular and orthopedic surgeons performs emergency surgery and controls the bleeding. Section of the humeral circumflex artery is proposed as a definitive diagnosis.
He evolved in the admission room at our institution, upon being evaluated by our team we found marked edema of the upper limb with a very weak pulse, very slow capillary refill, anesthesia of the upper limb, and significant hematoma in the wound area.
New emergency hematological complementary tests, emergency Doppler ultrasound and close clinical follow-up are proposed.
Acute anemia of 9.6 grL is found in the complementary patients, but flow is seen in the axillary artery on ultrasound. Figure 1.
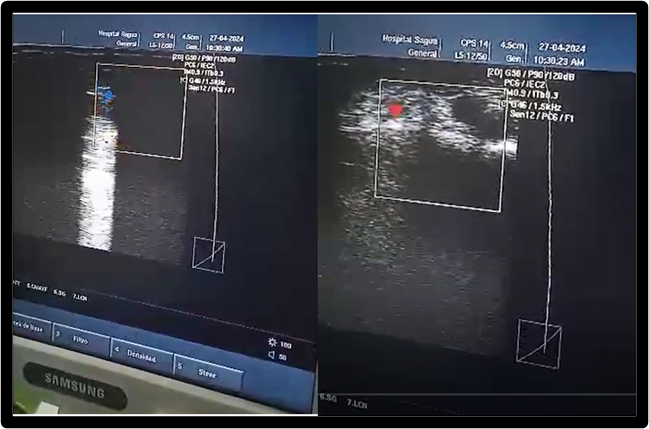
Figure 1: Flow is seen in the axillary artery on ultrasound.
When carrying out complementary evaluations (acute anemia 8.2grL) and collective analysis, it was decided to take the patient back to the operating room to explore the wound again. Also, on this occasion, the surgical group was made up of vascular, orthopedic, and anesthesia and resuscitation surgeons with extensive experience. in trauma management. Figure 2
An exploration of the wound made in the previous intervention is carried out and we collectively consider that it does not provide possibilities for
approaching the great vessels of the axillary area, we make an incision in the path of the axillary artery, we expose the area and active arterial bleeding is observed. Vascular control is performed, an end-to-end anastomosis is performed with Polyester 5.0 suture (Figure 3). We checked the brachial plexus nerves and there was no nerve injury. The muscular planes are faced, covering repair and sawing through planes up to the skin.
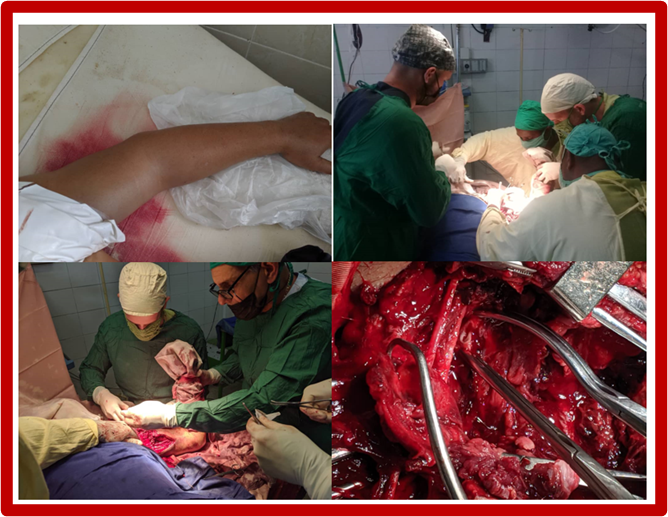
Figure 2. Note the edema of the upper limb, the surgical approach to the injury, the multidisciplinary team working, and finally the approximation of the edges of the axillary wound.
It should be noted that vascular repair is a determining factor for the viability of the limb, but its function is determined by the neurological injury and its repair.
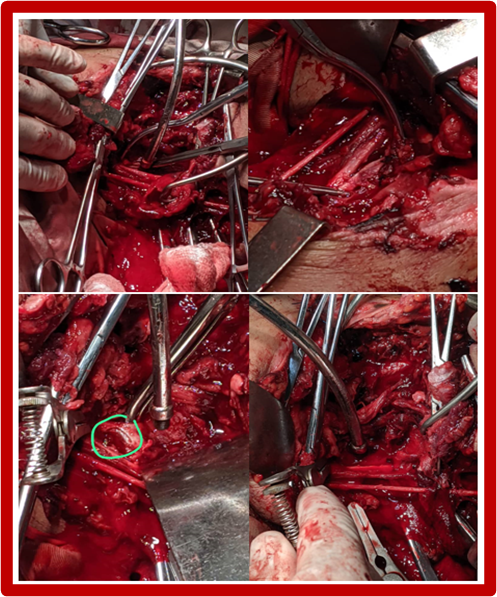
Figure 3. Exploration of the lesion, brachial plexus nerves without injuries, injury to the axillary artery and end of surgery with arterial suture
Major peripheral vascular trauma is defined as injuries to blood vessels (arterial and venous) greater than 4 mm; 3% of all trauma injuries have a vascular component. 2, 7 These injuries must be identified and managed efficiently, otherwise it can lead to the loss of a limb or even the patient's life. For this it is essential not to delay the diagnosis. Axillary artery injuries are relatively rare and may go unnoticed on initial evaluation. They represent less than 5% of all vascular lesions. Despite being a rare injury, 61-66% die on the way to receive medical attention and 23% upon arrival at the hospital [8].
Injury to the axillary artery is a rare entity with high mortality, usually secondary to penetrating trauma; It depends on factors such as trauma kinematics, patient morphology, and response time. Reconstruction of the. axillary artery with a cephalic vein graft compared to the saphenous vein reduces surgical time and the risk of new hematoma [9].
History Vascular trauma and the need to control bleeding have played an important role in the survival of humanity throughout history. The first known records of this practice date back to the years 1600 BC, when, according to the Ebers papyrus (discovered by Ebers in Luxor in 1873), mixtures of mineral oil or vegetable matter such as lead sulfate, antimony or copper sulfate They were used by the Egyptians to control bleeding. On the other hand, the Chinese in approximately 1000 BC described the use of tight bandages and metallized materials to control bleeding. Galen, in the 2nd century BC, referred to the need to differentiate venous bleeding from arterial bleeding, since he stated that in venous bleeding, compression or the application of certain materials was sufficient to control hemorrhage, but in the case of a arterial bleeding, ligation with linen was necessary. [10, 11].
Epidemiology Vascular trauma is considered a serious injury, it can progress to the amputation of a limb or the death of the patient. Of these, axillary artery injuries are rare, but represent less than 5% of all vascular traumas in civilians; however, despite their limited frequency, these injuries are associated with morbidity and mortality rates ranging from 5% to 39%.
Between 27% and 44 of axillary artery injuries are accompanied by brachial plexus injuries, the main indicator of long-term morbidity. Other concomitant injuries are axillary vein trauma in 30%-43% [12].
In Colombia, 0.67% of trauma admissions to the emergency department correspond to vascular injuries;3-6 this type of trauma, although it does not have a high incidence, is a major public health problem given its lethality and complications. [13, 14].
In Paraguay these cases are very rare according to Kunzle Elizeche,15 in Venezuela Sulbarán5 reports that peripheral vascular trauma was present in less than 5% of polytraumas, however, it is potentially lethal.
Vascular trauma in Mexico is a critical health problem, deaths from this cause are increasing, predominating in productive stages of life and constituting a challenge for the vascular surgeon, because patients always have a high potential for complications. Hence, their attention is and should be expeditious, in order to reduce complications and have a better percentage of good results. They report in their study that 79.3% are men, average age 36.2 years, with sharps injuries in 16.3% of those injured and 29.3% had upper limb injuries.[16].
Herrera reports that Mattox et al conducted a systematic review of patients with vascular trauma over 30 years, reporting a prevalence of vascular trauma of 14% in the upper extremities [17].
In Argentina, Soteras and collaborators present a 10-year study on traumatic vascular injuries, with 470 patients, of which 112 MMSS injuries were involved, the axillary artery was compromised in 22 patients (19.6%), 11 (50%) per room, 13 venous bypasses, 5 prosthetic bypasses and 4 end-to-end sutures were performed. Two patients presented serious neurological injury [18].
In Cuba, Cruz Lara and collaborator report a forensic medicine study on deaths in Havana, 3.44% were reported as a direct cause of a vascular injury; 48%, due to a knife. The blood vessels that were most frequently injured were: the aorta artery, the pulmonary artery and the vena cava. Six people died from vascular injuries to the extremities [19].
Positive diagnosis
The diagnosis of vascular lesions is made almost exclusively through history and physical examination, which upon completion must make a decision regarding the need to perform immediate operative exploration or observation and additional diagnostic tests. The absence of hard signs of vascular trauma almost 100% eliminates the possibility of vascular injury, but does not exclude it. Its presence is an indication for immediate exploration [12].
The diagnosis is purely clinical and is based on physical examination and sometimes complementary examinations. Hard signs such as bleeding or pulsating hematoma, absence of distal pulse and signs of acute ischemia are efficient in confirming vascular trauma with a positive predictive value of almost 100%, but their absence does not completely exclude it. Table 1
A pulse can be found in about a third of lesions since the arterial lumen is not completely compromised or is maintained thanks to the existing collateral circulation. axillary artery injuries given that there is an extensive network of anastomoses around the shoulder, which sometimes delays the diagnosis. In various case reports, the absence of a pulse was present in up to 20% of cases. When this occurs, soft signs should be looked for such as wound in the vicinity of the major vessels, transient bleeding after the accident, decreased distal pulses with low distal perfusion or formation of a non-pulsatile hematoma [12].
Ischemia occurs as a result of a sudden interruption of blood flow to the extremities, resulting in insufficient oxygen supply, giving way to the installation of anaerobic metabolism in the affected territory. Given the above, accumulation of lactic acid occurs along with inflammatory mediators, activating humoral and cellular inflammatory cascades, progressing to cell death if the oxygen supply is not recovered in a timely manner. Ischemia time greater than 6 hours is identified as a risk factor for amputation; Revascularizing before 6 hours after trauma is related to better postsurgical results and lower rates of limb loss [20].
| Hard signs | Soft signs |
| a) Pulsatile external hemorrhage. | a) Stable hematoma. |
| b) Murmur or thrill over the injured artery. | b) Unexplained transient hypotension. |
| c) Pulsatile hematoma. | c) Injury close to important vessels. |
| d) Ischemic signs: absence of pulses, pain, paleness, coldness, paresthesia and paralysis. | d) Neurological deficit. |
| e) Decrease in distal pulse. |
Table 1: Characteristic clinical signs of vascular lesions.
Ortega et al report that Ramírez-Morin reports that in 59.6% of cases with vascular injuries, hard signs of injury were found; Complementary imaging was performed in 25% of the patients prior to the surgical approach.21
There are other supportive diagnostic studies, but their usefulness is limited to the clinical stability of the patient according to the clinical signs presented at the time of evaluation, among which are: pulse oximetry, ITB, duplex Doppler ultrasound, angiotomography and angiography.
| Type of traumatic injury | Clinical signs |
| Complete section | Absence of distal pulses, limb ischemia |
| Partial section | Hemorrhage, hematoma, decreased pulse |
| Contusion | Initial examination may be normal, may progress to thrombosis |
| Pseudoaneurysm | The initial examination may be normal, presence of murmur or thrill, expansive pulse |
| Arteriovenous fistula | The initial examination may be normal, presence of murmur or thrill, decreased pulses |
| Extrinsic compression | Decreased pulses, recovery of normal pulses when the fracture is reduced |
Differential diagnosis
Table 2: Differential diagnoses of arterial trauma and their possible clinical signs.
Treatment The management priorities for this type of injury consist of stopping hemorrhage and restoring normal circulation, initially performing adequate resuscitation management, shock reversal, and hemorrhage control; to later, in the operating room, perform proximal and distal control of the injured vessel and identify the injury, decide the type of repair to be performed, which will fundamentally depend on the extent of the damage [22].
Regarding vascular repair techniques, one must choose between open surgery or endovascular technique, open surgery being the Gold Standard to date. A wide incision is recommended that allows adequate visualization for proximal and distal vascular control. [23].
In open trauma of the axillary artery, management is usually very complex, since active bleeding or tension hematoma are usually serious. To approach axillary injuries, it may be necessary to control the subclavian artery with an infraclavicular, and more rarely supraclavicular, incision; If the injury affects up to the thoracic outlet, the sub clavicular or direct axillary route is generally sufficient. Dissection of the axillary artery, given its fragility, must be extremely careful. Depending on the type of injury, we will use direct suture, an end-to-end anastomosis or inverted saphenous vein interposition.
Simultaneous reconstruction of the axillary vein is convenient, but if it is complex (need for graft), its ligation can be tolerated, due to the good collateral circulation in the area. If there are severed ends of the brachial plexus, we must mark them with non-absorbable sutures for delayed reconstruction.
Conservative treatment. Regarding the expectant treatment of non-symptomatic lesions, there are several groups with sufficient experience that publish good results in patients with minimal, non-occlusive and asymptomatic lesions. They must meet the following criteria: minimal injuries (less than 5 mm), with a minimal flap that does not compromise distal circulation and without active hemorrhage. In these cases, follow-up with color Doppler ultrasound is essential and has confirmed the stability and healing of the lesions [24, 26].
Treatment with endovascular techniques. Endovascular techniques are rarely useful in this sector [27].
Treatment with open arterial suture. The basic principle of vascular repair is to achieve proximal and distal control before addressing the damaged site. To achieve adequate proximal control, an incision must be made away from the bleeding site, in the same way as distal control (see figure 2). Small wounds with clear and transverse edges, partially affecting the circumference of the vessel, can be repaired with a primary suture. In case of larger defects, the possibility of stenosis after primary suture is high, so the use of sutures is preferable. vein patches or prosthetic materials. When it is not possible to free both ends or the wall loss is ≥1 cm, reverse vein grafting or the use of a prosthesis is preferred [28].
The Prospective Observational Vascular Injury Treatment (PROOVIT) registry collected 542 patients with vascular trauma, of whom 241 had peripheral vascular trauma. Conservative management was chosen in 33% of those in the upper limbs, an initial surgical approach was performed in 71% of those in the upper limbs, the primary repair rate was 78% [29].
Axillary arterial injuries can coexist with proximal humerus fractures, shoulder dislocations, and neurological damage to the brachial plexus [30].
Author's considerations
The analysis of cases promotes constant improvement in the quality of patient care, avoiding inappropriate management and complications. Addressing these considerations by the service is very necessary.
Vascular trauma can have serious consequences, such as amputation of a limb or death of the patient. Axillary artery injuries in the context of trauma are rare, their management requires a high index of suspicion, a multidisciplinary approach and adequate surgical access and management.