AUCTORES
Globalize your Research
Review Article | DOI: https://doi.org/10.31579/2578-8965/305
1Department of Obstetrics and Gynaecology, Nnamdi Azikiwe University Awka, Anambra State, Nigeria.
2Department of Obstetrics and Gynaecology, Nnamdi Azikiwe University Teaching Hospital, Nnewi, Anambra State, Nigeria.
3Department of Obstetrics and Gynaecology, Barking, Havering and Redbridge University Hospitals NHS, Romford, London.
4Division of Maternal Fetal Medicine, Department of Gynecology and Obstetrics, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
*Corresponding Author: George Uchenna Eleje., Department of Obstetrics and Gynaecology, Nnamdi Azikiwe University Awka, Anambra State, Nigeria.
Citation: Malarchy E. Nwankwo, Samuel N. Ugadu, Arinze C. Ikeotuonye, Richard O. Egeonu, George U. Eleje, et al, (2026), Premature Rupture of Fetal Membranes: A Narrative Review Integrating Current Evidence and International Guidelines for Optimal Care, J. Obstetrics Gynecology and Reproductive Sciences, 10(3) DOI:10.31579/2578-8965/305
Copyright: © 2026, George Uchenna Eleje. This is an open-access article distributed under the terms of The Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Received: 25 March 2026 | Accepted: 01 April 2026 | Published: 13 April 2026
Keywords: premature rupture of membranes; preterm premature rupture of membranes; preterm labour; preterm delivery; chorioamnionitis; cytokines
Premature rupture of fetal membranes (PROM) is a significant obstetric complication associated with preterm birth and increased maternal and neonatal morbidity and mortality, particularly in resource-limited settings. It is a multifactorial condition resulting from complex interactions between infectious, inflammatory, mechanical, and biochemical processes that weaken the chorioamniotic membranes. This narrative review synthesises current evidence and international clinical guidelines on the diagnosis and management of PROM. It examines the epidemiology, risk factors, and underlying pathophysiology, with emphasis on the roles of infection, inflammatory mediators, and matrix metalloproteinases. Diagnostic strategies are reviewed, including clinical assessment, conventional bedside tests, and emerging biomarker-based approaches such as placental alpha-microglobulin-1 and insulin-like growth factor binding protein-1. Evidence-based management approaches are discussed, including prophylactic antibiotics, antenatal corticosteroids, magnesium sulphate for fetal neuroprotection, selective use of tocolysis, and gestational age-specific timing of delivery. Emerging areas, including outpatient management, prevention strategies, amnioinfusion in preterm PROM, and considerations for cerclage retention and breech presentation, are also addressed. In conclusion, this review provides a comprehensive and up-to-date synthesis of current knowledge on PROM to inform clinical practice. Improved risk stratification, timely diagnosis, and adherence to evidence-based management remain essential to optimise maternal and neonatal outcomes.
Prelabour rupture of membranes (PROM) refers to rupture of the fetal membranes prior to the onset of uterine contractions and the establishment of labour[1]. Depending on the gestational age at which membrane rupture occurs, PROM is further classified into distinct clinical categories. When rupture occurs before the age of fetal viability, defined in many low-resource settings as 28 weeks of gestation, it is referred to as previable PROM. Rupture that occurs before 37 completed weeks of gestation is termed preterm PROM (PPROM), whereas term PROM refers to rupture of the membranes occurring at or beyond 37 weeks of gestation [1,2].
PROM represents a relatively common obstetric complication, affecting approximately 8–10% of all pregnancies worldwide [3]. The incidence of previable PROM is comparatively low, occurring in less than 1% of pregnancies, while PPROM complicates about 2–3% of pregnancies and accounts for nearly one-third of all preterm births (PTB).[1,2] PROM occurring at term constitutes the majority of cases, affecting approximately 8% of pregnancies. Overall, rupture of membranes occurs at term in nearly 80% of PROM cases. Following rupture at term, spontaneous labour typically ensues within a short period; approximately 60% of women go into labour within 24 hours, and up to 95?gin labour within 72 hours of membrane rupture.[4]
Data from local clinical settings also highlight the burden of PROM. In a five-year retrospective review involving 3,513 deliveries at the Nnamdi Azikiwe University Teaching Hospital (NAUTH), Nigeria, Eleje et al. reported an incidence of 2.4% for term PROM [5]. These findings emphasize the continued relevance of PROM as a significant obstetric condition that contributes to both maternal and neonatal morbidity (Figure 1).
This narrative review examines the epidemiology, risk factors, and aetiopathogenesis of premature rupture of fetal membranes (PROM), with particular emphasis on the roles of infection, inflammatory cytokines, and matrix metalloproteinases in membrane weakening and rupture. It further evaluates contemporary diagnostic approaches, including clinical assessment, conventional bedside tests, and emerging biomarker-based methods such as placental alpha-microglobulin-1 and insulin-like growth factor binding protein-1. Finally, the review synthesises current evidence and international clinical guidelines to inform the optimal management of PROM.
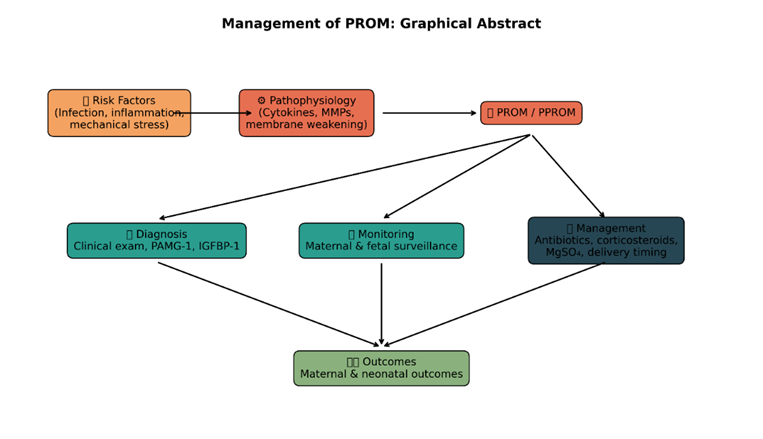
Figure 1: Schematic management of PROM
Search strategy
A comprehensive and systematic literature search was conducted to identify relevant studies, guidelines, and evidence relating to the management of premature rupture of fetal membranes. The search process was guided by a structured query formulated as “Recent guidelines for management of premature rupture of fetal membranes.” This query was designed to capture the most up-to-date and clinically relevant publications addressing diagnosis, risk factors, complications, and management strategies for PROM.
Multiple electronic databases and information sources were explored to ensure broad coverage of the available literature. These included PubMed, Google Scholar, ResearchGate, Scopus, Web of Science, the Cochrane Library, and general Google searches, as well as relevant clinical protocols and international guideline documents. A wide range of keywords and search phrases were used either singly or in combination. These included premature rupture of fetal membranes, preterm premature rupture of fetal membranes, term premature rupture of fetal membranes, previable premature rupture of fetal membranes, chorioamnionitis, preterm labor, preterm delivery, inflammatory cytokines in labor, recent evidence for diagnosing premature rupture of fetal membranes, complications of premature rupture of fetal membranes, and management of premature rupture of fetal membranes.
Following the initial search, older publications with limited relevance to current clinical practice were excluded. A total of 123 publications were initially identified. After screening for relevance and methodological suitability, 92 publications were selected for detailed review and citation in this narrative review. Selection of the final references was based on their relevance to the research objectives, contribution to contemporary understanding of PROM, and applicability to clinical practice.
Risk factors for PROM
A previous history of PROM represents the most significant and consistently reported risk factor for recurrence in subsequent pregnancies.[6] Aris et al. documented a recurrence risk of 6.6% among women with a prior history of PROM.[7] Evidence from a large prospective observational study conducted by the National Institute of Child Health and Human Development Maternal-Fetal Medicine Units Research Network further supports this association. In that study, 13.5% of women with a history of preterm birth resulting from PROM experienced PROM in a subsequent pregnancy, compared with 4.1% among women without a prior history of PROM, corresponding to a risk ratio (RR) of 3.3 (95% confidence interval [CI], 2.1–5.2).[8,9]
In addition to a prior history, several maternal, obstetric, and environmental factors have been associated with an increased risk of PROM. Genetic collagen vascular disorders, including Ehlers-Danlos syndrome, systemic lupus erythematosus, and Marfan syndrome, can compromise the structural integrity of the fetal membranes. Structural abnormalities of the uterus, cervical insufficiency, and previous cervical surgical procedures such as conization and loop electrosurgical excision procedure (LEEP) also contribute to membrane weakness and subsequent rupture [10,11].
Infectious and inflammatory conditions of the urogenital tract, as well as periodontal disease, have also been implicated in the pathogenesis of PROM. Other recognised obstetric risk factors include uterine overdistension resulting from polyhydramnios or multiple gestations, abdominal trauma, antepartum haemorrhage, and invasive prenatal diagnostic procedures such as amniocentesis, chorionic villus sampling, and cordocentesis. Environmental and socioeconomic factors further contribute to risk, including malnutrition, maternal anemia, low body mass index (BMI), cigarette smoking, and low socioeconomic status. [10,11]
More recently, Lin et al. conducted a systematic review and meta-analysis involving 21 studies and 18,174 women, which identified several additional factors significantly associated with PROM. These included low BMI, short interpregnancy interval (IPI <2 years), previous abortion, prior preterm birth, previous PROM, history of caesarean section, gestational hypertension, gestational diabetes mellitus, abnormal vaginal discharge, reproductive tract infections, fetal malpresentation, and increased abdominal pressure.[12] These findings underscore the multifactorial nature of PROM and the importance of identifying both modifiable and non-modifiable risk factors in clinical practice.
Aetiopathogenesis of PROM
The aetiology of PROM is multifactorial, and the precise pathophysiologic mechanisms underlying membrane rupture remain incompletely understood. A central feature of PROM is disruption of the collagen framework of the chorioamniotic membranes, which compromises membrane strength and predisposes to rupture. Infectious and inflammatory processes play a major role in this collagen remodeling process.
Collagen vascular disorders can predispose women to PROM by altering the structural composition and mechanical integrity of the fetal membranes, which are largely composed of collagen. During intrauterine infection or inflammation, bacterial products and pro-inflammatory cytokines, particularly interleukin-1 beta (IL-1β) and tumour necrosis factor-alpha (TNF-α), stimulate the production of prostaglandins and increase the expression of matrix metalloproteinases (MMPs), also referred to as collagenases. These enzymes degrade the collagen matrix of the chorioamniotic membranes, leading to progressive weakening and eventual rupture.[11]
Biochemical studies have provided further insight into these mechanisms. Maymon et al. reported that PPROM is associated with increased amniotic fluid concentrations of MMP-1 and MMP-8 [13,14]. In addition, Maymon et al. and Athayde et al. demonstrated that women with microbial invasion of the amniotic cavity exhibit significantly higher concentrations of MMP-9 compared with women without microbial invasion[15,16].
Microbial infection has also been shown to play a significant role in PROM. Eleje et al. examined 210 endocervical swabs obtained from 105 women with PROM and 105 controls matched for age, parity, and gestational age [17]. Their findings revealed a significantly higher microbial culture positivity rate of 79.05% among cases compared with 6.67% among controls (p <0.05). Among the microorganisms identified, Streptococcus species were the most frequently isolated pathogens, occurring in 31.43% of cases compared with 4.81% of controls. Conversely, Candida albicans was significantly more prevalent in controls (27.62% vs 8.57%). Additionally, Gardnerella vaginalis and Trichomonas vaginalis were significantly more common among women with PPROM than among women with intact membranes.[17]
Periodontal disease has also been implicated in the pathogenesis of PROM. This condition represents a chronic inflammatory disorder of the supporting structures of the teeth and is dominated by gram-negative anaerobic bacteria. PROM may occur when oral bacteria gain access to the systemic circulation through bacterial invasion of the dental pulp following cavitation in untreated dental disease.[18]
Mechanical factors also contribute to membrane rupture. Mechanical stretching of the membranes, resulting from preterm uterine contractions or uterine overdistension in conditions such as polyhydramnios and multiple gestations, may weaken the membranes and predispose them to rupture. Additionally, fetal membranes may be iatrogenically ruptured during invasive procedures, including amniocentesis, chorionic villus sampling, and cordocentesis.[11]
Diagnosis of PROM
In most cases, the diagnosis of PROM is made clinically. Approximately 90% of women present with a characteristic history of a sudden gush of fluid from the vagina followed by continuous leakage, which strongly suggests rupture of the membranes [19]. The diagnosis is confirmed when amniotic fluid is seen passing through the cervical os and/or when pooling of fluid is observed in the posterior vaginal fornix during sterile speculum examination [20]. Speculum examination also provides an opportunity to assess for cervical dilatation and effacement, cervicitis, and umbilical cord prolapse, and to obtain samples for microbiological studies where indicated. By contrast, digital vaginal examination should be avoided, unless the speculum findings suggest marked cervical dilatation, labour is established, or delivery appears imminent. This precaution is important because digital examination has been associated with increased risks of chorioamnionitis, neonatal infection, and shortened latency [3,20-22]. Since speculum assessment correlates well with digital findings in the evaluation of the cervix [23], it is generally sufficient in most clinical settings.
Despite the usefulness of history and examination, the diagnosis remains uncertain in about 10–20% of cases, necessitating the use of adjunctive tests. Traditional bedside tests include the nitrazine test and ferning test. A blue colour change on nitrazine paper and arborization on microscopy support the diagnosis of PROM; however, their diagnostic value is limited by false-positive results caused by semen, cervical mucus, blood, cervicitis, vaginitis, alkaline urine, and topical antiseptics [19,20]. The fetal fibronectin test is highly sensitive but lacks specificity for PROM. A negative result strongly suggests intact membranes, whereas a positive result does not establish the diagnosis with certainty. Accordingly, fetal fibronectin is more useful as a predictor of preterm birth than as a primary diagnostic test for PROM [24].
More invasive diagnostic procedures have also been described. In women with suspected PROM, amniocentesis followed by instillation of indigo carmine dye into the amniotic cavity may confirm rupture if blue-stained fluid leaks vaginally within 20–30 minutes. Although this method is diagnostically useful, it is invasive, costly, and associated with risks including iatrogenic PROM, placental abruption, infection, and miscarriage. The use of methylene blue is especially problematic because of its association with fetal hemolytic jaundice, hemolytic anaemia, hyperbilirubinaemia, and methemoglobinemia [25]. For these reasons, amnio-dye testing should not be used routinely in the diagnosis of PROM. Ultrasonography may demonstrate oligohydramnios, which can support the clinical impression, but it should not be used in isolation to establish the diagnosis. Its more important role lies in the assessment of fetal well-being, fetal presentation, placental location, estimated fetal weight, structural anomalies, and residual amniotic fluid volume [26].
When the diagnosis is equivocal, biochemical marker tests in vaginal secretions have emerged as valuable tools. These include placental alpha-microglobulin-1 (PAMG-1; AmniSure), insulin-like growth factor binding protein-1 (IGFBP-1; Actim PROM), and alpha-fetoprotein (AFP). Studies have shown these tests to be superior to conventional clinical methods in difficult cases [27,28]. Ibrahim et al. reported that the Amnioquick Duo+ test, which detects IGFBP-1 and AFP, had significantly greater diagnostic accuracy than both nitrazine and fern tests in identifying PROM [29]. In a comparative study, Eleje et al. found that Amnioquick Duo+ and PAMG-1 demonstrated similarly high diagnostic performance in equivocal cases, with a concordance rate of 97.0% [30]. In a meta-analysis, Palacio et al. showed that Actim PROM and AmniSure had comparable sensitivity (95.4% vs 96.7%) and negative predictive value (95.8% vs 96.7%), although AmniSure had higher specificity (98.3% vs 92.9%) and positive predictive value (98.3% vs 92.3%) [31]. In practical terms, PROM is unlikely when there is no clinical evidence of amniotic fluid leakage or pooling and PAMG-1 or IGFBP-1 testing is negative [32].
Diagnosis of chorioamnionitis following PROM
Chorioamnionitis, whether diagnosed clinically or histologically, is a major complication of PROM and is reported in 30–80% of preterm births associated with PPROM [33]. Its diagnosis remains challenging because the clinical manifestations are often nonspecific and may overlap with other maternal or fetal conditions. The cardinal clinical signs include maternal fever (≥100.4°F), maternal tachycardia (>100 beats/min), fetal tachycardia (>160 beats/min), uterine tenderness, and purulent or foul-smelling vaginal discharge [3]. Diagnostic criteria vary across clinical practice. Some clinicians consider the presence of any two clinical features sufficient for diagnosis, while others require fever plus at least two additional signs, a stricter definition that appears to improve diagnostic accuracy [34,35]. Among these features, fever is the most sensitive, occurring in 95–100% of cases. Maternal tachycardia and fetal tachycardia show sensitivities of 50–80% and 40–70%, respectively, whereas uterine tenderness and offensive vaginal discharge are more subjective and are present in only 4–25% of cases [35].
Because clinical features alone lack specificity, laboratory evaluation is often used to support diagnosis. Leukocytosis (>12,000–15,000/mm3) is found in 70–90% of cases, but it is a weak standalone marker because elevated white cell counts may also occur in normal pregnancy, labour, and other pathological states [35]. Similarly, cardiotocography and the fetal biophysical profile perform poorly in predicting chorioamnionitis after PROM [36]. Caloone et al. reported that C-reactive protein (CRP) was the best maternal serum marker for predicting chorioamnionitis in PROM [37], but Sabogal et al. found only modest diagnostic performance, with a sensitivity of 68.7% and specificity of 77.1% [38]. Eleje et al. evaluated interleukin-6 (IL-6) in cervicovaginal secretions using the Chorioquick test and demonstrated its potential clinical utility in detecting chorioamnionitis in women with PROM [39]. Nevertheless, a systematic review and meta-analysis by Etyang et al. concluded that there remains insufficient evidence to support routine use of CRP, procalcitonin, or IL-6 as reliable diagnostic markers for chorioamnionitis in PROM [40].
Taken together, the available evidence indicates that neither clinical signs nor laboratory markers are sufficiently sensitive or specific when used in isolation. Therefore, current recommendations favour a combined diagnostic approach, integrating clinical findings with relevant laboratory parameters when evaluating women with PROM for possible chorioamnionitis [3,32].
| Authors | Maternal age (years) | Parity | Gestational age (weeks) | Clinical presentation | Specific investigation findings | Treatment | Gestational age at delivery | Mode of delivery | Feto-maternal outcome |
| Early et al.41 | 35 years | G4P2+1 | 13 weeks plus 3 days | Leakage of fluid per vagina following CVS. VE: Positive pooling, nitrazine, and ferning test. | U/SS: Oligohydramnios. | Expectant management. Patient reported no drainage of liquor on the 3rd day. | 36 weeks | Elective induction of labor/vaginal delivery. | Live female neonate, that weighed 2.7kg with good APGAR score. |
| Hidalgo-Chicharro et al.42 | 26 years | G3P2 | 32 weeks | Discharge of clear fluid per vagina. VE: Closed cervix with clear fluid in the vagina. | U/SS: Viable singleton fetus with adequate liquor volume, | Conservative management: Antibiotics, steroid, | 33 weeks plus 4 days | Induction of labor/vaginal delivery | Live female baby that weighed 1.8kg with good APGAR Scores. Admitted in NICU and subsequently discharged. |
| Ekpa et al.43 | 30 years | G2P1 | 29weeks plus 6days | Leakage of fluid per vagina of 2 hours duration. VE: Pool of liquor in posterior vaginal fornix, liquor trickling down an open cervical os on valsalva maneuver | U/SS: Viable pregnancy with severe oligohydramnios (AFI = 0.8cm) | Conservative management: Antibiotics, tocolysis, steroid, bed rest, | 30 weeks plus 2 days. | Emergency caesarean section. | Live 1.4kg female neonate .with good APGAR score. Baby was subsequently discharged after two weeks from the SCBU. Mother had pneumonia and was treated appropriately and discharged. |
| Alkasseh et al.44 | 32 years | G4P3 | 32weeks | Discharge of clear fluid per vagina. VE: Speculum shows pool of liquor in the posterior fornix, | U/SS: Closed cervix, adequate liquor, | Conservative management: Antibiotics, steroid, tocolysis. | 33 weeksplus 4 days. | Vaginal delivery following induction of labor. | Live female neonate that weighed 1.97kg with good APGAR score. Subsequently discharged on 13th day post-delivery from NICU. |
| Jha et al.45 | 25 years | Primigravida | 20 weeks | Drainage of liquor per vagina. VE: Speculum shows pool on liquor in the vagina. | U/SS: AFI of 9.4cm and 3.2cm on first and fourth day. | Expectant management: Antibiotics, pelvic rest, Subsequently discharged 10th day on admission following cessation of liquor. | 37 weeks | Caesarean delivery | Live 3.2kgmale baby with satisfactory APGAR score. Mother was stable. |
| Shaheed et al.46 | Not mentioned | Primigravida | 28 | Watery vaginal discharge of 2 weeks duration. VE: closedcervix, liquor trickling down the cervix. | U/SS: Viable singleton pregnancy at 31+ weeks with moderate oligohydraminous. | Antibiotics, hormonal support, and steroid | 32 weeks | Emergency caesarean section | Healthy, live 2.7kg female baby with good APGAR score. Baby subsequently discharged from NICU following phototherapy on account of neonatal jaundice. |
| Chmaj-Wierzchowska et al.47 | 27 | Primipara | 19weeks | Profuse vaginal discharge x 2 weeks. VE: Closed cervix, subsequent speculum examination revealed pool of amniotic fluid in the vagina | U/ss: Normal for gestational age fetus, oligohydramnios, elevated CRP, positive vaginal culture | Initial intravaginal suppository antibiotics, Magnesium hydoaspartate, drotaverine hydrochloride, Betamethasone, | 31/32weeks | Caesarean section | Live 1.2kg male baby. Discharged subsequently in good condition |
| Wu et al.48 | 32 years | Primigravida | 18 weeks | Drainage of fluid per vagina following amniocentesis on account of positive maternal serum screening for down syndrome in a twin pregnancy. | U/SS: Nearly no liquor for twin B. | Antibiotics, tocolytics | 30 weeks plus 2days | Emergency Caesarean section due to abruptio placenta | Live twin babies that weighed 1.5kg (Twin A) and 0.83kg (Twin B). Both twin had PDA, received ventilation support. Twin B had severe IUGR and IVH, and subsequently died. |
Table 1: Summary of cases of premature rupture of fetal membranes (PROM).
VE = Vaginal examination, U/SS = Ultrasonography, IVH = Intra-ventricular haemorrhage, IUGR = Intra-uterine growth restriction, PDA = Patent ductus arteriosus, AFI = Amniotic fluid index, NICU = Neonatal intensive care unit
Antibiotic prophylaxis following PROM
Administration of prophylactic antibiotics after PROM has been shown to reduce both maternal and neonatal morbidity. Documented benefits include lower rates of chorioamnionitis, neonatal infection, surfactant use, neonatal intensive care unit admission, and neonatal cerebral abnormalities, together with prolongation of the latency period [49]. Recommended regimens vary slightly across professional bodies. The National Institute for Health and Care Excellence (NICE) recommends oral erythromycin 250 mg four times daily for up to 10 days or until established labour, whichever occurs first [32]. This recommendation is largely based on the ORACLE I trial, which demonstrated more favourable maternal and neonatal outcomes with erythromycin than with co-amoxiclav alone or co-amoxiclav combined with erythromycin [50].
By contrast, the American College of Obstetricians and Gynaecologists (ACOG) recommends the regimen used in the National Institute of Child Health and Human Development Maternal–Fetal Medicine Units Network trial, consisting of intravenous ampicillin 2 g every 6 hours plus erythromycin 250 mg every 6 hours for 48 hours, followed by oral amoxicillin 250 mg every 8 hours and erythromycin base 333 mg every 8 hours for 5 days [51]. The Society of Obstetricians and Gynaecologists of Canada (SOGC) accepts either of these regimens [52]. Importantly, co-amoxiclav should be avoided because of its association with necrotizing enterocolitis in the neonate [50].
Corticosteroid use in women with PROM
Antenatal corticosteroids remain a key component of care in women with PROM who are at risk of preterm birth. Their use reduces neonatal mortality and major neonatal morbidity, particularly intraventricular haemorrhage and respiratory distress syndrome, without increasing the risk of chorioamnionitis or neonatal infection [53]. The WHO Action Trial, which assessed the safety and effectiveness of antenatal glucocorticoids in low-resource settings, found that among women at risk of preterm birth, dexamethasone significantly reduced stillbirth and neonatal death without increasing maternal bacterial infection [54]. A Cochrane review of 12 trials involving 1,557 women and 1,661 infants found that dexamethasone and betamethasone had comparable efficacy [55]. In most of the head-to-head trials, two 12 mg intramuscular doses of betamethasone given 24 hours apart were compared with four 6 mg intramuscular doses of dexamethasone given 12 hours apart, and ACOG endorses either regimen [56].
A single course of antenatal corticosteroids is recommended for women with PROM between 24+0 and 33+6 weeks of gestation when delivery is considered likely within the next 7 days [20,32,56]. Although routine steroid use in the late preterm period (34+0 to 36+6 weeks) has traditionally been approached cautiously because of the risk of neonatal hypoglycaemia, findings from the Antenatal Late Preterm Steroids (ALPS) trial, a multicentre randomized study involving 2,831 women in 17 centres, showed that steroids given before anticipated late preterm delivery significantly reduced respiratory distress syndrome, stillbirth, and neonatal death within 72 hours of birth [57]. Since the optimal benefit of corticosteroids extends for approximately 7 days, a single repeat course may be considered in women at less than 34 weeks’ gestation if more than 7 days have passed since the initial course and there is a high likelihood of preterm birth within 48 hours [32]. More than two courses should not be administered, given the adverse effects of repeated exposure on fetal growth and neurodevelopment [53].
Administration of magnesium sulphate in women with PROM
The fetal neuroprotective role of antenatal magnesium sulphate in women with PPROM is well established. A Cochrane review including five trials and 6,145 babies showed that magnesium sulphate administered to women at risk of preterm birth significantly reduced the likelihood of cerebral palsy and gross motor dysfunction [58]. Although different dosing schedules were used across the included trials, there is no clear evidence favouring one specific regimen [59]. Most guidelines therefore recommend using the minimum effective dose to reduce the risk of toxicity. The most widely recommended approach consists of a 4 g intravenous loading dose given slowly over 15–30 minutes, followed by a maintenance infusion of 1 g/hour until birth or for a maximum of 24 hours, whichever occurs first [32,60,61].
In low-resource settings where continuous intravenous infusion may not be feasible because of staffing or monitoring limitations, an alternative regimen may be used: 4 g intravenously over 20–30 minutes, followed by 5 g intramuscularly into each buttock, and then 5 g intramuscularly into alternate buttocks every 4 hours for 24 hours [3]. Regardless of the regimen, women receiving magnesium sulphate require close clinical monitoring. Pulse rate, blood pressure, respiratory rate, and deep tendon reflexes should be assessed at least every 4 hours [32,61]. Treatment should be stopped if signs of toxicity develop, including absent patellar reflexes, respiratory rate below 12/minute, a diastolic blood pressure drop greater than 15 mmHg below baseline, or urine output below 100 mL over 4 hours [3]. Calcium gluconate should be readily available as an antidote. Current guidance recommends magnesium sulphate for women with PROM at risk of preterm birth between 24+0 and 33+6 weeks of gestation [32,60,61]. There is no evidence supporting repeat dosing after a completed initial course [3].
Use of tocolytics in women with PROM
The role of tocolysis in women with PPROM remains limited. A Cochrane review of eight trials involving 408 women found that although tocolytic therapy prolonged latency and reduced birth within 48 hours, it was also associated with a higher frequency of 5-minute Apgar score <7, increased need for neonatal ventilation, and a significantly increased risk of chorioamnionitis [62]. On this basis, routine tocolysis is not recommended in women with PPROM, as the maternal infectious risk outweighs the uncertain neonatal benefit [63].
That said, short-term tocolysis for up to 48 hours may be considered in selected women with PPROM at less than 34 weeks’ gestation, mainly to permit completion of antenatal corticosteroids and/or facilitate in-utero transfer to a facility with appropriate neonatal care [63,64]. When tocolysis is indicated, nifedipine or atosiban are preferred first-line agents because they offer similar efficacy and perinatal outcomes [64]. A commonly recommended nifedipine schedule is an initial dose of 10–30 mg, followed by 10–20 mg every 4–8 hours until contractions cease or for a maximum of 48 hours [65]. Betamimetics should be avoided because of their potentially severe cardiovascular adverse effects [66]. If one agent fails, a second drug from a different class may be used, but combination tocolysis is not recommended [65,66].
Timing of delivery in women with PROM
Previable PROM (<28 weeks of gestation)
Previable PROM is associated with substantial maternal and neonatal risk. A recent systematic review and meta-analysis of 19 studies involving 1,640 singleton pregnancies showed that expectant management after previable or periviable PROM was associated with high rates of spontaneous abortion, fetal demise, maternal chorioamnionitis, endometritis, neonatal sepsis, and neonatal death [67]. Smaller observational studies by Beydoun et al., Sim et al., and Fernandes et al. reported similarly poor outcomes [34,68,69]. In view of these risks, women with previable PROM should receive clear counselling regarding the prognosis of expectant management and should be offered termination of pregnancy [20]. For women who choose expectant management, counselling should be repeated and comprehensive, antibiotic therapy should be given, and antenatal corticosteroids should be administered once the pregnancy reaches viability. Tocolysis is not recommended in this group [20].
Preterm PROM (28+0 to 36+6 weeks of gestation)
Management of PPROM in the viable preterm period depends largely on gestational age and the balance between the hazards of prematurity and the risks of intrauterine infection. In a systematic review and meta-analysis of five randomized controlled trials including 488 women, Al-Mandeel et al. compared expectant management with immediate delivery between 28 and 34 weeks of gestation. Rates of maternal infection, respiratory distress syndrome, and neonatal sepsis were similar between the two groups; however, neonatal death and caesarean section were significantly more frequent in the immediate-delivery group [70]. These findings indicate that immediate birth between 28 and 34 weeks confers no added benefit and may worsen important maternal and neonatal outcomes. In uncomplicated PPROM during this gestational window, expectant management reduces prematurity-related morbidity, and ACOG recommends continuation of pregnancy until 34 weeks, provided no contraindication arises [20].
Historically, immediate delivery was advised for women with PPROM between 34+0 and 36+6 weeks [1,71]. More recent evidence has modified this approach. Current guidance supports offering expectant management until 37 weeks in the absence of contraindications to continuing the pregnancy [63]. This shift is based on the Cochrane review by Bond et al., which compared planned early birth with expectant management in women with PPROM before 37 weeks and found no reduction in neonatal sepsis with early delivery. Instead, early delivery was associated with increased risks of respiratory distress syndrome, need for ventilation, neonatal intensive care unit admission, neonatal mortality, endometritis, induction of labour, and caesarean birth [72]. Follow-up evidence on behavioural and neurodevelopmental outcomes at 2 years of age found no difference between infants delivered after expectant management and those delivered immediately following late PPROM [73]. Together, these data support a more conservative strategy in stable women.
PROM at term
At term, the clinical context differs because the fetus is mature and the major concern shifts toward prevention of ascending infection. Approximately 60% of women with term PROM enter spontaneous labour within 24 hours, and 95% do so within 72 hours [4]. A meta-analysis by Mozurkewich and Wolf, which included 23 studies and 7,493 women, found no difference in caesarean delivery or neonatal infection rates between immediate induction and conservative management, but showed lower rates of chorioamnionitis and endometritis with induction [74]. Similarly, a randomized controlled trial by Awakadigwe et al. reported that although active and expectant management produced comparable delivery modes and complication rates, active management significantly reduced both the latency period and the induction-to-delivery interval [75]. In the same meta-analysis, induction with vaginal prostaglandins was associated with more chorioamnionitis than oxytocin induction [74]. In the absence of contraindications, vaginal birth remains the preferred route of delivery for PROM beyond 28 weeks, as it is associated with less maternal and perinatal morbidity than caesarean delivery [76].
Home/outpatient management of women with PROM
The role of outpatient management in women with PPROM remains incompletely defined because the supporting evidence is limited and heterogeneous. Dussaux et al. conducted a retrospective cohort study of 90 women with PPROM between 24 and 34 weeks managed at home and compared them with 324 women managed in hospital. They found that outpatient care was not associated with major maternal or neonatal complications [77]. Likewise, Carlan et al. performed a randomized controlled trial in which 67 women with PPROM were allocated to either home-based or hospital-based management, and they reported no significant differences in perinatal outcomes between the two groups [78]. However, a Cochrane review comparing home versus hospital management for PPROM at less than 37 weeks identified only two small studies, both of which were underpowered to detect clinically important differences [79]. As such, the current evidence base is insufficient to support routine outpatient care for all women with PROM.
This uncertainty is reflected in current clinical guidance. The most recent Royal College of Obstetricians and Gynaecologists (RCOG) guideline is the first major guideline to explicitly address outpatient management and recommends that the decision should be individualized. It further acknowledges that factors influencing latency to delivery should be taken into account and that the optimal monitoring strategy for predicting adverse fetal outcomes after PPROM remains uncertain [63,80]. By contrast, ACOG, in guidance published one year later, does not support outpatient care during the viable period, citing insufficient evidence regarding safety.
Even in settings where outpatient care is offered selectively, important uncertainties remain regarding the frequency, content, and effectiveness of surveillance. Hall et al. recently examined monitoring practices, clinical outcomes, and patient experience in women with PPROM managed as outpatients [81]. Their study collected retrospective data on demographic characteristics, baseline risk factors, diagnostic details, outpatient monitoring practices, maternal observations, biochemical tests, ultrasound findings, delivery outcomes, and placental histopathology [81]. Counselling practices were also evaluated both at diagnosis and during the first consultant review, and women were invited to participate in a service evaluation regarding their care experience. Across six participating units, 233 women with PPROM were managed in outpatient services. The median gestational age at diagnosis was 32 weeks, and around 34% of diagnoses were equivocal. The study found marked variation across centres in the counselling provided regarding pregnancy outcomes [81]. Spontaneous preterm birth occurred in 41% of women, while an additional 18% required preterm delivery for suspected chorioamnionitis. All participating units used maternal pulse rate, temperature, CRP, and white cell count to assess infection, but neither the absolute values at delivery nor their change over time predicted histological chorioamnionitis. Although most women considered outpatient care acceptable, many reported insufficient emotional support during management [81]. These findings suggest that outpatient care may be feasible for carefully selected women, but standardized monitoring pathways and supportive care frameworks are still needed.
Prediction and prevention of PROM
Efforts to identify reliable predictors of PROM have generated interest in a range of biochemical and hematologic markers, although no test has yet entered routine clinical use. Underhill et al. suggested that maternal serum biglycan, decorin, and sex hormone-binding globulin (SHBG) may have potential as predictive markers of PPROM in otherwise asymptomatic women [82]. Other studies have explored additional candidate markers, including elevated second-trimester maternal serum amyloid A, increased platelet-to-lymphocyte ratio (PLR), increased neutrophil-to-lymphocyte ratio (NLR), and placental protein 14 [83-85]. While these biomarkers are of research interest, their predictive performance has not been sufficiently validated for routine clinical application.
Preventive strategies have focused primarily on addressing known risk factors. Modifiable factors include cessation of cigarette smoking, prompt treatment of urogenital, respiratory, and periodontal infections, and amnioreduction in women with polyhydramnios to decrease excessive uterine distension [6]. Management of non-modifiable or partially modifiable risk states may include vaginal progesterone and cerclage in women with a short cervix or a history of previous preterm birth [6]. Woods et al. proposed that reactive oxygen species may contribute to PROM and suggested vitamin C and E supplementation as possible preventive interventions [86]. However, higher-quality evidence has not supported the effectiveness of such approaches. In a systematic review and meta-analysis, El-Achi et al. evaluated 29 studies examining 10 interventions, including docosahexaenoic acid (DHA), aspirin, rofecoxib, vitamin C alone or combined with vitamin E, folic acid in different formulations, zinc, calcium, copper, and treatment of bacterial vaginosis [87]. They concluded that none of these interventions significantly reduced the incidence of PPROM. At present, no biomarker or preventive strategy can be recommended as a proven method for reliably predicting or preventing PROM.
Amnioinfusion in the management of PPROM
Amnioinfusion, used to restore amniotic fluid volume, has been investigated as a potential intervention in PPROM. A Cochrane review by Hofmeyr et al found that transcervical amnioinfusion improved fetal umbilical artery pH and reduced variable decelerations, while transabdominal amnioinfusion was associated with reductions in neonatal death, sepsis, pulmonary hypoplasia, and puerperal infection [88]. However, these findings were based on a small number of trials and were largely influenced by a single study with methodological limitations, warranting cautious interpretation. Similarly, a meta-analysis by Celik et al evaluating serial transabdominal amnioinfusion in early PPROM demonstrated prolongation of latency and improved long-term survival in observational studies, although these benefits were not consistently confirmed in randomised trials [89]. Overall, current evidence remains limited and inconclusive, and routine use of amnioinfusion in PPROM cannot be recommended pending further high-quality randomised controlled trials [88, 89].
Removal versus retention of cerclage in preterm premature rupture of membranes
Cervical cerclage is an established intervention for preventing preterm birth but is associated with complications such as PPROM and chorioamnionitis [90, 91]. The optimal timing of cerclage removal following PPROM remains debated. Evidence from a meta-analysis by Zullo et al suggests that immediate removal reduces latency but is associated with lower rates of chorioamnionitis and adverse neonatal outcomes, highlighting a trade-off between prolonging pregnancy and infection risk [90]. A pragmatic approach involves short-term retention (approximately 24 hours) to allow completion of antenatal corticosteroid therapy, followed by removal, thereby balancing neonatal benefits and infection risks [91]. However, findings across studies remain inconsistent. Current guidance, supported by Ghareeb et al, recommends expectant management with cerclage retention until 32–34 weeks’ gestation in the absence of labour, infection, or bleeding [91]. Further robust evidence is needed to guide optimal management.
PROM and breech presentation
Evidence on term premature rupture of membranes (PROM) in breech presentation is limited, despite clinical concerns regarding cord prolapse and infection risk. Evidence on term PROM in breech presentation remains limited, despite concerns about cord prolapse and infection. Rasch et al conducted a prospective cohort study of 2876 women with singleton breech presentation, including 1920 planned vaginal deliveries (642 PROM; 1278 spontaneous rupture of membranes [SROM]) [92]. No significant differences were observed in maternal or neonatal outcomes between PROM and SROM groups, including comparable modified PREMODA scores [92]. However, PROM was associated with slightly higher maternal body mass index and increased use of epidural analgesia. It was concluded that PROM does not appear to worsen outcomes in term breech deliveries when managed by experienced clinicians, supporting management approaches similar to cephalic presentations while maintaining vigilance for cord prolapse in selected cases [92].
Premature rupture of membranes (PROM) remains a significant obstetric challenge due to its contribution to preterm birth and associated neonatal morbidity and mortality. A prior history of PROM is the strongest risk factor, highlighting the importance of risk stratification. Diagnosis is primarily clinical, with adjunctive tests such as PAMG-1 and IGFBP-1 reserved for equivocal cases. Management is guided by gestational age and the balance between infection and prematurity risks, incorporating antibiotics, antenatal corticosteroids, and magnesium sulphate for fetal neuroprotection before 34 weeks. Tocolysis is not routinely recommended but may be used short term for specific indications. Expectant management is generally appropriate for preterm PROM in the absence of contraindications, while active management is preferred at term. Currently, no reliable strategies exist for the prediction or prevention of PROM. Emerging approaches, including outpatient care and amnioinfusion, remain investigational. Clinical decision-making should also consider complexities such as cerclage retention and PROM in breech presentation, while exercising caution in the interpretation of diagnostic tests in uncertain cases.
Author contribution
M.E. Nwankwo, S.N. Ugadu, A.C. Ikeotuonye, R.O. Egeonu, E.I. Ogumu, were involved in conceptualization, manuscript writing. C.G. Okafor, B.O. Nwosu, G.U. Eleje, C.A .Okeke; and A.C. Eke were involved in manuscript writing and revision. All authors participated in manuscript revision. All authors approved the final copy for submission to the journal.
Ethical approval
Not applicable
Declaration of conflicting interest
The authors declare no competing interest.
Funding
Except for the sole purpose of disseminating scientific knowledge, the authors received no funding or any financial inducement to publish this review of literature.
Informed Consent
Not applicable
Data availability statement
Not applicable
Acknowledgement
The authors would like to express their gratitude to everyone that participated in this review article. Additionally, we are grateful to the scholars whose works we have consulted and cited for this evaluation.
PROM = Premature Rupture of foetal Membranes
PPROM = Preterm PROM
PTB = Preterm Birth
IVH = Intraventricular Haemorrhage
IUGR = Intrauterine Growth Restriction
PDF = Patent Ductus Arteriosus
AFI = Amniotic Fluid Index
NICU = Neonatal Intensive Care Unit
NAUTH = Nnamdi Azikiwe University Teachng Hospital
RR = Relative Risk
CI = Confidence Interval
BMI = Body Mass Index
IPI = Inter Pregnancy Interval
GDM = Gestational Diabetes Mellitus
DHA = Docasahexaenoic Acd
IL-1β = Interleukin 1 beta
TNF-α = Tumour necrosis factor alpha
ALPS = Antenatal Late Preterm Steroids
RCT = Randomized Controlled Trial
RDS = Respiratory Distress Syndrom
SHBG = Sex Hormone Binding Globulin
PLR = Platelet-to-lymphocyte ratio
NLR = Neutrophil-to-lymphocyte ratio
NICE = National Institute for Health and Care Excellence
ORACLE = Overview of the Role of Antibiotics in Curtailing Labour and Early delivery
ACOG = American College of Obstetricians and Gynaecologists
SOGC = Society of Obstetricians and Gynaecologists of Canada
WHO = World Health Organisation
IL-6 = Interleukin 6
MMP = Matrix Metalloproteinases
PAMG-1 = Placental alpha microglobulin-1
IGFBP-1 = Insulin-like growth factor binding protein-1
AFP = Alpha-fetoprotein
CRP = C-reactive protein.
Clearly Auctoresonline and particularly Psychology and Mental Health Care Journal is dedicated to improving health care services for individuals and populations. The editorial boards' ability to efficiently recognize and share the global importance of health literacy with a variety of stakeholders. Auctoresonline publishing platform can be used to facilitate of optimal client-based services and should be added to health care professionals' repertoire of evidence-based health care resources.

Journal of Clinical Cardiology and Cardiovascular Intervention The submission and review process was adequate. However I think that the publication total value should have been enlightened in early fases. Thank you for all.

Journal of Women Health Care and Issues By the present mail, I want to say thank to you and tour colleagues for facilitating my published article. Specially thank you for the peer review process, support from the editorial office. I appreciate positively the quality of your journal.
Journal of Clinical Research and Reports I would be very delighted to submit my testimonial regarding the reviewer board and the editorial office. The reviewer board were accurate and helpful regarding any modifications for my manuscript. And the editorial office were very helpful and supportive in contacting and monitoring with any update and offering help. It was my pleasure to contribute with your promising Journal and I am looking forward for more collaboration.

We would like to thank the Journal of Thoracic Disease and Cardiothoracic Surgery because of the services they provided us for our articles. The peer-review process was done in a very excellent time manner, and the opinions of the reviewers helped us to improve our manuscript further. The editorial office had an outstanding correspondence with us and guided us in many ways. During a hard time of the pandemic that is affecting every one of us tremendously, the editorial office helped us make everything easier for publishing scientific work. Hope for a more scientific relationship with your Journal.

The peer-review process which consisted high quality queries on the paper. I did answer six reviewers’ questions and comments before the paper was accepted. The support from the editorial office is excellent.

Journal of Neuroscience and Neurological Surgery. I had the experience of publishing a research article recently. The whole process was simple from submission to publication. The reviewers made specific and valuable recommendations and corrections that improved the quality of my publication. I strongly recommend this Journal.

Dr. Katarzyna Byczkowska My testimonial covering: "The peer review process is quick and effective. The support from the editorial office is very professional and friendly. Quality of the Clinical Cardiology and Cardiovascular Interventions is scientific and publishes ground-breaking research on cardiology that is useful for other professionals in the field.

Thank you most sincerely, with regard to the support you have given in relation to the reviewing process and the processing of my article entitled "Large Cell Neuroendocrine Carcinoma of The Prostate Gland: A Review and Update" for publication in your esteemed Journal, Journal of Cancer Research and Cellular Therapeutics". The editorial team has been very supportive.

Testimony of Journal of Clinical Otorhinolaryngology: work with your Reviews has been a educational and constructive experience. The editorial office were very helpful and supportive. It was a pleasure to contribute to your Journal.

Dr. Bernard Terkimbi Utoo, I am happy to publish my scientific work in Journal of Women Health Care and Issues (JWHCI). The manuscript submission was seamless and peer review process was top notch. I was amazed that 4 reviewers worked on the manuscript which made it a highly technical, standard and excellent quality paper. I appreciate the format and consideration for the APC as well as the speed of publication. It is my pleasure to continue with this scientific relationship with the esteem JWHCI.

This is an acknowledgment for peer reviewers, editorial board of Journal of Clinical Research and Reports. They show a lot of consideration for us as publishers for our research article “Evaluation of the different factors associated with side effects of COVID-19 vaccination on medical students, Mutah university, Al-Karak, Jordan”, in a very professional and easy way. This journal is one of outstanding medical journal.
Dear Hao Jiang, to Journal of Nutrition and Food Processing We greatly appreciate the efficient, professional and rapid processing of our paper by your team. If there is anything else we should do, please do not hesitate to let us know. On behalf of my co-authors, we would like to express our great appreciation to editor and reviewers.

As an author who has recently published in the journal "Brain and Neurological Disorders". I am delighted to provide a testimonial on the peer review process, editorial office support, and the overall quality of the journal. The peer review process at Brain and Neurological Disorders is rigorous and meticulous, ensuring that only high-quality, evidence-based research is published. The reviewers are experts in their fields, and their comments and suggestions were constructive and helped improve the quality of my manuscript. The review process was timely and efficient, with clear communication from the editorial office at each stage. The support from the editorial office was exceptional throughout the entire process. The editorial staff was responsive, professional, and always willing to help. They provided valuable guidance on formatting, structure, and ethical considerations, making the submission process seamless. Moreover, they kept me informed about the status of my manuscript and provided timely updates, which made the process less stressful. The journal Brain and Neurological Disorders is of the highest quality, with a strong focus on publishing cutting-edge research in the field of neurology. The articles published in this journal are well-researched, rigorously peer-reviewed, and written by experts in the field. The journal maintains high standards, ensuring that readers are provided with the most up-to-date and reliable information on brain and neurological disorders. In conclusion, I had a wonderful experience publishing in Brain and Neurological Disorders. The peer review process was thorough, the editorial office provided exceptional support, and the journal's quality is second to none. I would highly recommend this journal to any researcher working in the field of neurology and brain disorders.

Dear Agrippa Hilda, Journal of Neuroscience and Neurological Surgery, Editorial Coordinator, I trust this message finds you well. I want to extend my appreciation for considering my article for publication in your esteemed journal. I am pleased to provide a testimonial regarding the peer review process and the support received from your editorial office. The peer review process for my paper was carried out in a highly professional and thorough manner. The feedback and comments provided by the authors were constructive and very useful in improving the quality of the manuscript. This rigorous assessment process undoubtedly contributes to the high standards maintained by your journal.

International Journal of Clinical Case Reports and Reviews. I strongly recommend to consider submitting your work to this high-quality journal. The support and availability of the Editorial staff is outstanding and the review process was both efficient and rigorous.

Thank you very much for publishing my Research Article titled “Comparing Treatment Outcome Of Allergic Rhinitis Patients After Using Fluticasone Nasal Spray And Nasal Douching" in the Journal of Clinical Otorhinolaryngology. As Medical Professionals we are immensely benefited from study of various informative Articles and Papers published in this high quality Journal. I look forward to enriching my knowledge by regular study of the Journal and contribute my future work in the field of ENT through the Journal for use by the medical fraternity. The support from the Editorial office was excellent and very prompt. I also welcome the comments received from the readers of my Research Article.

Dear Erica Kelsey, Editorial Coordinator of Cancer Research and Cellular Therapeutics Our team is very satisfied with the processing of our paper by your journal. That was fast, efficient, rigorous, but without unnecessary complications. We appreciated the very short time between the submission of the paper and its publication on line on your site.

I am very glad to say that the peer review process is very successful and fast and support from the Editorial Office. Therefore, I would like to continue our scientific relationship for a long time. And I especially thank you for your kindly attention towards my article. Have a good day!

"We recently published an article entitled “Influence of beta-Cyclodextrins upon the Degradation of Carbofuran Derivatives under Alkaline Conditions" in the Journal of “Pesticides and Biofertilizers” to show that the cyclodextrins protect the carbamates increasing their half-life time in the presence of basic conditions This will be very helpful to understand carbofuran behaviour in the analytical, agro-environmental and food areas. We greatly appreciated the interaction with the editor and the editorial team; we were particularly well accompanied during the course of the revision process, since all various steps towards publication were short and without delay".

I would like to express my gratitude towards you process of article review and submission. I found this to be very fair and expedient. Your follow up has been excellent. I have many publications in national and international journal and your process has been one of the best so far. Keep up the great work.

We are grateful for this opportunity to provide a glowing recommendation to the Journal of Psychiatry and Psychotherapy. We found that the editorial team were very supportive, helpful, kept us abreast of timelines and over all very professional in nature. The peer review process was rigorous, efficient and constructive that really enhanced our article submission. The experience with this journal remains one of our best ever and we look forward to providing future submissions in the near future.

I am very pleased to serve as EBM of the journal, I hope many years of my experience in stem cells can help the journal from one way or another. As we know, stem cells hold great potential for regenerative medicine, which are mostly used to promote the repair response of diseased, dysfunctional or injured tissue using stem cells or their derivatives. I think Stem Cell Research and Therapeutics International is a great platform to publish and share the understanding towards the biology and translational or clinical application of stem cells.

I would like to give my testimony in the support I have got by the peer review process and to support the editorial office where they were of asset to support young author like me to be encouraged to publish their work in your respected journal and globalize and share knowledge across the globe. I really give my great gratitude to your journal and the peer review including the editorial office.

I am delighted to publish our manuscript entitled "A Perspective on Cocaine Induced Stroke - Its Mechanisms and Management" in the Journal of Neuroscience and Neurological Surgery. The peer review process, support from the editorial office, and quality of the journal are excellent. The manuscripts published are of high quality and of excellent scientific value. I recommend this journal very much to colleagues.

Dr.Tania Muñoz, My experience as researcher and author of a review article in The Journal Clinical Cardiology and Interventions has been very enriching and stimulating. The editorial team is excellent, performs its work with absolute responsibility and delivery. They are proactive, dynamic and receptive to all proposals. Supporting at all times the vast universe of authors who choose them as an option for publication. The team of review specialists, members of the editorial board, are brilliant professionals, with remarkable performance in medical research and scientific methodology. Together they form a frontline team that consolidates the JCCI as a magnificent option for the publication and review of high-level medical articles and broad collective interest. I am honored to be able to share my review article and open to receive all your comments.

“The peer review process of JPMHC is quick and effective. Authors are benefited by good and professional reviewers with huge experience in the field of psychology and mental health. The support from the editorial office is very professional. People to contact to are friendly and happy to help and assist any query authors might have. Quality of the Journal is scientific and publishes ground-breaking research on mental health that is useful for other professionals in the field”.

Dear editorial department: On behalf of our team, I hereby certify the reliability and superiority of the International Journal of Clinical Case Reports and Reviews in the peer review process, editorial support, and journal quality. Firstly, the peer review process of the International Journal of Clinical Case Reports and Reviews is rigorous, fair, transparent, fast, and of high quality. The editorial department invites experts from relevant fields as anonymous reviewers to review all submitted manuscripts. These experts have rich academic backgrounds and experience, and can accurately evaluate the academic quality, originality, and suitability of manuscripts. The editorial department is committed to ensuring the rigor of the peer review process, while also making every effort to ensure a fast review cycle to meet the needs of authors and the academic community. Secondly, the editorial team of the International Journal of Clinical Case Reports and Reviews is composed of a group of senior scholars and professionals with rich experience and professional knowledge in related fields. The editorial department is committed to assisting authors in improving their manuscripts, ensuring their academic accuracy, clarity, and completeness. Editors actively collaborate with authors, providing useful suggestions and feedback to promote the improvement and development of the manuscript. We believe that the support of the editorial department is one of the key factors in ensuring the quality of the journal. Finally, the International Journal of Clinical Case Reports and Reviews is renowned for its high- quality articles and strict academic standards. The editorial department is committed to publishing innovative and academically valuable research results to promote the development and progress of related fields. The International Journal of Clinical Case Reports and Reviews is reasonably priced and ensures excellent service and quality ratio, allowing authors to obtain high-level academic publishing opportunities in an affordable manner. I hereby solemnly declare that the International Journal of Clinical Case Reports and Reviews has a high level of credibility and superiority in terms of peer review process, editorial support, reasonable fees, and journal quality. Sincerely, Rui Tao.

Clinical Cardiology and Cardiovascular Interventions I testity the covering of the peer review process, support from the editorial office, and quality of the journal.

Clinical Cardiology and Cardiovascular Interventions, we deeply appreciate the interest shown in our work and its publication. It has been a true pleasure to collaborate with you. The peer review process, as well as the support provided by the editorial office, have been exceptional, and the quality of the journal is very high, which was a determining factor in our decision to publish with you.
The peer reviewers process is quick and effective, the supports from editorial office is excellent, the quality of journal is high. I would like to collabroate with Internatioanl journal of Clinical Case Reports and Reviews journal clinically in the future time.

Clinical Cardiology and Cardiovascular Interventions, I would like to express my sincerest gratitude for the trust placed in our team for the publication in your journal. It has been a true pleasure to collaborate with you on this project. I am pleased to inform you that both the peer review process and the attention from the editorial coordination have been excellent. Your team has worked with dedication and professionalism to ensure that your publication meets the highest standards of quality. We are confident that this collaboration will result in mutual success, and we are eager to see the fruits of this shared effort.

Dear Dr. Jessica Magne, Editorial Coordinator 0f Clinical Cardiology and Cardiovascular Interventions, I hope this message finds you well. I want to express my utmost gratitude for your excellent work and for the dedication and speed in the publication process of my article titled "Navigating Innovation: Qualitative Insights on Using Technology for Health Education in Acute Coronary Syndrome Patients." I am very satisfied with the peer review process, the support from the editorial office, and the quality of the journal. I hope we can maintain our scientific relationship in the long term.
Dear Monica Gissare, - Editorial Coordinator of Nutrition and Food Processing. ¨My testimony with you is truly professional, with a positive response regarding the follow-up of the article and its review, you took into account my qualities and the importance of the topic¨.

Dear Editorial Coordinator of the Journal of Nutrition and Food Processing! "I would like to thank the Journal of Nutrition and Food Processing for including and publishing my article. The peer review process was very quick, movement and precise. The Editorial Board has done an extremely conscientious job with much help, valuable comments and advices. I find the journal very valuable from a professional point of view, thank you very much for allowing me to be part of it and I would like to participate in the future!”

Dealing with The Journal of Neurology and Neurological Surgery was very smooth and comprehensive. The office staff took time to address my needs and the response from editors and the office was prompt and fair. I certainly hope to publish with this journal again.Their professionalism is apparent and more than satisfactory. Susan Weiner

My Testimonial Covering as fellowing: Lin-Show Chin. The peer reviewers process is quick and effective, the supports from editorial office is excellent, the quality of journal is high. I would like to collabroate with Internatioanl journal of Clinical Case Reports and Reviews.

My experience publishing in Psychology and Mental Health Care was exceptional. The peer review process was rigorous and constructive, with reviewers providing valuable insights that helped enhance the quality of our work. The editorial team was highly supportive and responsive, making the submission process smooth and efficient. The journal's commitment to high standards and academic rigor makes it a respected platform for quality research. I am grateful for the opportunity to publish in such a reputable journal.
My experience publishing in International Journal of Clinical Case Reports and Reviews was exceptional. I Come forth to Provide a Testimonial Covering the Peer Review Process and the editorial office for the Professional and Impartial Evaluation of the Manuscript.

I would like to offer my testimony in the support. I have received through the peer review process and support the editorial office where they are to support young authors like me, encourage them to publish their work in your esteemed journals, and globalize and share knowledge globally. I really appreciate your journal, peer review, and editorial office.
Dear Agrippa Hilda- Editorial Coordinator of Journal of Neuroscience and Neurological Surgery, "The peer review process was very quick and of high quality, which can also be seen in the articles in the journal. The collaboration with the editorial office was very good."

I would like to express my sincere gratitude for the support and efficiency provided by the editorial office throughout the publication process of my article, “Delayed Vulvar Metastases from Rectal Carcinoma: A Case Report.” I greatly appreciate the assistance and guidance I received from your team, which made the entire process smooth and efficient. The peer review process was thorough and constructive, contributing to the overall quality of the final article. I am very grateful for the high level of professionalism and commitment shown by the editorial staff, and I look forward to maintaining a long-term collaboration with the International Journal of Clinical Case Reports and Reviews.
To Dear Erin Aust, I would like to express my heartfelt appreciation for the opportunity to have my work published in this esteemed journal. The entire publication process was smooth and well-organized, and I am extremely satisfied with the final result. The Editorial Team demonstrated the utmost professionalism, providing prompt and insightful feedback throughout the review process. Their clear communication and constructive suggestions were invaluable in enhancing my manuscript, and their meticulous attention to detail and dedication to quality are truly commendable. Additionally, the support from the Editorial Office was exceptional. From the initial submission to the final publication, I was guided through every step of the process with great care and professionalism. The team's responsiveness and assistance made the entire experience both easy and stress-free. I am also deeply impressed by the quality and reputation of the journal. It is an honor to have my research featured in such a respected publication, and I am confident that it will make a meaningful contribution to the field.

"I am grateful for the opportunity of contributing to [International Journal of Clinical Case Reports and Reviews] and for the rigorous review process that enhances the quality of research published in your esteemed journal. I sincerely appreciate the time and effort of your team who have dedicatedly helped me in improvising changes and modifying my manuscript. The insightful comments and constructive feedback provided have been invaluable in refining and strengthening my work".

I thank the ‘Journal of Clinical Research and Reports’ for accepting this article for publication. This is a rigorously peer reviewed journal which is on all major global scientific data bases. I note the review process was prompt, thorough and professionally critical. It gave us an insight into a number of important scientific/statistical issues. The review prompted us to review the relevant literature again and look at the limitations of the study. The peer reviewers were open, clear in the instructions and the editorial team was very prompt in their communication. This journal certainly publishes quality research articles. I would recommend the journal for any future publications.

Dear Jessica Magne, with gratitude for the joint work. Fast process of receiving and processing the submitted scientific materials in “Clinical Cardiology and Cardiovascular Interventions”. High level of competence of the editors with clear and correct recommendations and ideas for enriching the article.

We found the peer review process quick and positive in its input. The support from the editorial officer has been very agile, always with the intention of improving the article and taking into account our subsequent corrections.

My article, titled 'No Way Out of the Smartphone Epidemic Without Considering the Insights of Brain Research,' has been republished in the International Journal of Clinical Case Reports and Reviews. The review process was seamless and professional, with the editors being both friendly and supportive. I am deeply grateful for their efforts.
To Dear Erin Aust – Editorial Coordinator of Journal of General Medicine and Clinical Practice! I declare that I am absolutely satisfied with your work carried out with great competence in following the manuscript during the various stages from its receipt, during the revision process to the final acceptance for publication. Thank Prof. Elvira Farina

Dear Jessica, and the super professional team of the ‘Clinical Cardiology and Cardiovascular Interventions’ I am sincerely grateful to the coordinated work of the journal team for the no problem with the submission of my manuscript: “Cardiometabolic Disorders in A Pregnant Woman with Severe Preeclampsia on the Background of Morbid Obesity (Case Report).” The review process by 5 experts was fast, and the comments were professional, which made it more specific and academic, and the process of publication and presentation of the article was excellent. I recommend that my colleagues publish articles in this journal, and I am interested in further scientific cooperation. Sincerely and best wishes, Dr. Oleg Golyanovskiy.

Dear Ashley Rosa, Editorial Coordinator of the journal - Psychology and Mental Health Care. " The process of obtaining publication of my article in the Psychology and Mental Health Journal was positive in all areas. The peer review process resulted in a number of valuable comments, the editorial process was collaborative and timely, and the quality of this journal has been quickly noticed, resulting in alternative journals contacting me to publish with them." Warm regards, Susan Anne Smith, PhD. Australian Breastfeeding Association.

Dear Jessica Magne, Editorial Coordinator, Clinical Cardiology and Cardiovascular Interventions, Auctores Publishing LLC. I appreciate the journal (JCCI) editorial office support, the entire team leads were always ready to help, not only on technical front but also on thorough process. Also, I should thank dear reviewers’ attention to detail and creative approach to teach me and bring new insights by their comments. Surely, more discussions and introduction of other hemodynamic devices would provide better prevention and management of shock states. Your efforts and dedication in presenting educational materials in this journal are commendable. Best wishes from, Farahnaz Fallahian.
Dear Maria Emerson, Editorial Coordinator, International Journal of Clinical Case Reports and Reviews, Auctores Publishing LLC. I am delighted to have published our manuscript, "Acute Colonic Pseudo-Obstruction (ACPO): A rare but serious complication following caesarean section." I want to thank the editorial team, especially Maria Emerson, for their prompt review of the manuscript, quick responses to queries, and overall support. Yours sincerely Dr. Victor Olagundoye.

Dear Ashley Rosa, Editorial Coordinator, International Journal of Clinical Case Reports and Reviews. Many thanks for publishing this manuscript after I lost confidence the editors were most helpful, more than other journals Best wishes from, Susan Anne Smith, PhD. Australian Breastfeeding Association.

Dear Agrippa Hilda, Editorial Coordinator, Journal of Neuroscience and Neurological Surgery. The entire process including article submission, review, revision, and publication was extremely easy. The journal editor was prompt and helpful, and the reviewers contributed to the quality of the paper. Thank you so much! Eric Nussbaum, MD
Dr Hala Al Shaikh This is to acknowledge that the peer review process for the article ’ A Novel Gnrh1 Gene Mutation in Four Omani Male Siblings, Presentation and Management ’ sent to the International Journal of Clinical Case Reports and Reviews was quick and smooth. The editorial office was prompt with easy communication.

Dear Erin Aust, Editorial Coordinator, Journal of General Medicine and Clinical Practice. We are pleased to share our experience with the “Journal of General Medicine and Clinical Practice”, following the successful publication of our article. The peer review process was thorough and constructive, helping to improve the clarity and quality of the manuscript. We are especially thankful to Ms. Erin Aust, the Editorial Coordinator, for her prompt communication and continuous support throughout the process. Her professionalism ensured a smooth and efficient publication experience. The journal upholds high editorial standards, and we highly recommend it to fellow researchers seeking a credible platform for their work. Best wishes By, Dr. Rakhi Mishra.

Dear Jessica Magne, Editorial Coordinator, Clinical Cardiology and Cardiovascular Interventions, Auctores Publishing LLC. The peer review process of the journal of Clinical Cardiology and Cardiovascular Interventions was excellent and fast, as was the support of the editorial office and the quality of the journal. Kind regards Walter F. Riesen Prof. Dr. Dr. h.c. Walter F. Riesen.

Dear Ashley Rosa, Editorial Coordinator, International Journal of Clinical Case Reports and Reviews, Auctores Publishing LLC. Thank you for publishing our article, Exploring Clozapine's Efficacy in Managing Aggression: A Multiple Single-Case Study in Forensic Psychiatry in the international journal of clinical case reports and reviews. We found the peer review process very professional and efficient. The comments were constructive, and the whole process was efficient. On behalf of the co-authors, I would like to thank you for publishing this article. With regards, Dr. Jelle R. Lettinga.

Dear Clarissa Eric, Editorial Coordinator, Journal of Clinical Case Reports and Studies, I would like to express my deep admiration for the exceptional professionalism demonstrated by your journal. I am thoroughly impressed by the speed of the editorial process, the substantive and insightful reviews, and the meticulous preparation of the manuscript for publication. Additionally, I greatly appreciate the courteous and immediate responses from your editorial office to all my inquiries. Best Regards, Dariusz Ziora

Dear Chrystine Mejia, Editorial Coordinator, Journal of Neurodegeneration and Neurorehabilitation, Auctores Publishing LLC, We would like to thank the editorial team for the smooth and high-quality communication leading up to the publication of our article in the Journal of Neurodegeneration and Neurorehabilitation. The reviewers have extensive knowledge in the field, and their relevant questions helped to add value to our publication. Kind regards, Dr. Ravi Shrivastava.

Dear Clarissa Eric, Editorial Coordinator, Journal of Clinical Case Reports and Studies, Auctores Publishing LLC, USA Office: +1-(302)-520-2644. I would like to express my sincere appreciation for the efficient and professional handling of my case report by the ‘Journal of Clinical Case Reports and Studies’. The peer review process was not only fast but also highly constructive—the reviewers’ comments were clear, relevant, and greatly helped me improve the quality and clarity of my manuscript. I also received excellent support from the editorial office throughout the process. Communication was smooth and timely, and I felt well guided at every stage, from submission to publication. The overall quality and rigor of the journal are truly commendable. I am pleased to have published my work with Journal of Clinical Case Reports and Studies, and I look forward to future opportunities for collaboration. Sincerely, Aline Tollet, UCLouvain.

Dear Ms. Mayra Duenas, Editorial Coordinator, International Journal of Clinical Case Reports and Reviews. “The International Journal of Clinical Case Reports and Reviews represented the “ideal house” to share with the research community a first experience with the use of the Simeox device for speech rehabilitation. High scientific reputation and attractive website communication were first determinants for the selection of this Journal, and the following submission process exceeded expectations: fast but highly professional peer review, great support by the editorial office, elegant graphic layout. Exactly what a dynamic research team - also composed by allied professionals - needs!" From, Chiara Beccaluva, PT - Italy.

Dear Maria Emerson, Editorial Coordinator, we have deeply appreciated the professionalism demonstrated by the International Journal of Clinical Case Reports and Reviews. The reviewers have extensive knowledge of our field and have been very efficient and fast in supporting the process. I am really looking forward to further collaboration. Thanks. Best regards, Dr. Claudio Ligresti
Dear Chrystine Mejia, Editorial Coordinator, Journal of Neurodegeneration and Neurorehabilitation. “The peer review process was efficient and constructive, and the editorial office provided excellent communication and support throughout. The journal ensures scientific rigor and high editorial standards, while also offering a smooth and timely publication process. We sincerely appreciate the work of the editorial team in facilitating the dissemination of innovative approaches such as the Bonori Method.” Best regards, Dr. Matteo Bonori.

I recommend without hesitation submitting relevant papers on medical decision making to the International Journal of Clinical Case Reports and Reviews. I am very grateful to the editorial staff. Maria Emerson was a pleasure to communicate with. The time from submission to publication was an extremely short 3 weeks. The editorial staff submitted the paper to three reviewers. Two of the reviewers commented positively on the value of publishing the paper. The editorial staff quickly recognized the third reviewer’s comments as an unjust attempt to reject the paper. I revised the paper as recommended by the first two reviewers.

Dear Maria Emerson, Editorial Coordinator, Journal of Clinical Research and Reports. Thank you for publishing our case report: "Clinical Case of Effective Fetal Stem Cells Treatment in a Patient with Autism Spectrum Disorder" within the "Journal of Clinical Research and Reports" being submitted by the team of EmCell doctors from Kyiv, Ukraine. We much appreciate a professional and transparent peer-review process from Auctores. All research Doctors are so grateful to your Editorial Office and Auctores Publishing support! I amiably wish our article publication maintained a top quality of your International Scientific Journal. My best wishes for a prosperity of the Journal of Clinical Research and Reports. Hope our scientific relationship and cooperation will remain long lasting. Thank you very much indeed. Kind regards, Dr. Andriy Sinelnyk Cell Therapy Center EmCell

Dear Editorial Team, Clinical Cardiology and Cardiovascular Interventions. It was truly a rewarding experience to work with the journal “Clinical Cardiology and Cardiovascular Interventions”. The peer review process was insightful and encouraging, helping us refine our work to a higher standard. The editorial office offered exceptional support with prompt and thoughtful communication. I highly value the journal’s role in promoting scientific advancement and am honored to be part of it. Best regards, Meng-Jou Lee, MD, Department of Anesthesiology, National Taiwan University Hospital.

Dear Editorial Team, Journal-Clinical Cardiology and Cardiovascular Interventions, “Publishing my article with Clinical Cardiology and Cardiovascular Interventions has been a highly positive experience. The peer-review process was rigorous yet supportive, offering valuable feedback that strengthened my work. The editorial team demonstrated exceptional professionalism, prompt communication, and a genuine commitment to maintaining the highest scientific standards. I am very pleased with the publication quality and proud to be associated with such a reputable journal.” Warm regards, Dr. Mahmoud Kamal Moustafa Ahmed

Dear Maria Emerson, Editorial Coordinator of ‘International Journal of Clinical Case Reports and Reviews’, I appreciate the opportunity to publish my article with your journal. The editorial office provided clear communication during the submission and review process, and I found the overall experience professional and constructive. Best regards, Elena Salvatore.

Dear Mayra Duenas, Editorial Coordinator of ‘International Journal of Clinical Case Reports and Reviews Herewith I confirm an optimal peer review process and a great support of the editorial office of the present journal
Dear Editorial Team, Clinical Cardiology and Cardiovascular Interventions. I am really grateful for the peers review; their feedback gave me the opportunity to reflect on the message and impact of my work and to ameliorate the article. The editors did a great job in addition by encouraging me to continue with the process of publishing.

Dear Cecilia Lilly, Editorial Coordinator, Endocrinology and Disorders, Thank you so much for your quick response regarding reviewing and all process till publishing our manuscript entitled: Prevalence of Pre-Diabetes and its Associated Risk Factors Among Nile College Students, Sudan. Best regards, Dr Mamoun Magzoub.

International Journal of Clinical Case Reports and Reviews is a high quality journal that has a clear and concise submission process. The peer review process was comprehensive and constructive. Support from the editorial office was excellent, since the administrative staff were responsive. The journal provides a fast and timely publication timeline.

Dear Mayra Duenas, Editorial Coordinator of the journal IJCCR, I write here a little on my experience as an author submitting to the International Journal of Clinical Case Reports and Reviews (IJCCR). This was my first submission to IJCCR and my manuscript was inherently an outsider’s effort. It attempted to broadly identify and then make some sense of life’s under-appreciated mysteries. I initially had responded to a request for possible submissions. I then contacted IJCCR with a tentative topic for a manuscript. They quickly got back with an approval for the submission, but with a particular requirement that it be medically relevant. I then put together a manuscript and submitted it. After the usual back-and-forth over forms and formality, the manuscript was sent off for reviews. Within 2 weeks I got back 4 reviews which were both helpful and also surprising. Surprising in that the topic was somewhat foreign to medical literature. My subsequent updates in response to the reviewer comments went smoothly and in short order I had a series of proofs to evaluate. All in all, the whole publication process seemed outstanding. It was both helpful in terms of the paper’s content and also in terms of its efficient and friendly communications. Thank you all very much. Sincerely, Ted Christopher, Rochester, NY.

Dear Grace Pierce, Editorial Coordinator of the journal IJCCR, I had a very positive experience with Auctores - Journal throughout the publication process. The Editorial Team was highly responsive, professional, and supportive at every stage. I would like to extend my sincere thanks to the Editor: Grace Pierce, for her guidance and assistance. The peer-review process was smooth and constructive, helping improve the quality of my work. I would gladly recommend Auctores Journal to fellow researchers and authors. Dr. SABITA SINHA, Medical Oncologist, MD (Electro Homeopathy).

Dear Maria Emerson, Editorial Coordinator of - Journal of Clinical Research and Reports. ''I am pleased to provide this testimonial following the publication of our recent case report in this journal. The peer review process was rigorous, constructive, thorough, and conducted in a timely manner. The reviewers’ comments were thoughtful, detailed, and highly constructive, contributing substantially to the refinement, clarity, and scientific robustness of our manuscript. The process was conducted with professionalism and academic integrity throughout. The support provided by the editorial office was exemplary. Communication was consistently prompt, clear, and courteous at all stages of the submission and publication process. The editorial team demonstrated a high level of organization and responsiveness, ensuring that all queries were addressed efficiently and that the process remained transparent and well-coordinated. The overall quality of the journal is reflected in its strong editorial standards, commitment to scientific excellence, and dedication to publishing clinically meaningful research. It has been a privilege to publish our work in this journal, and we would welcome the opportunity to contribute further in the future.'' Best wishes from, Dr. Efstratios Trogkanis, Cardiologist.
Dear Reader: We have published several articles in the Auctores Publishing, LLC, journal, Clinical Medical Reviews and Reports in recent years (CMRR). This is an ‘open access’ journal and the following are our observations. From the initial invitation to submit an article, to the final edits of galley proofs, we have found CMRR personnel to be professional, responsive, rapid and thorough. This entire process begins with Catherine Mitchell, Editorial Coordinator. She is simply outstanding, and, I believe, unparalleled in her capacity. I cannot imagine a more responsive and dedicated Editorial Coordinator. As I read the dates and timing of her correspondence with us, it seems that she never sleeps. I hope Auctores Publishing, LLC, appreciates her efforts as much as these authors do. Thank you to Auctores Publishing, LLC, to the Editorial Staff/Board, and to Catherine Mitchell from a grateful author(s).

Dear Maria Emerson, Editorial Coordinator of International Journal of Clinical Case Reports and Reviews, What distinguishes International Journal of Clinical Case Report and Review is not only the scientific rigor of its publications, but the intellectual climate in which research is evaluated. The submission process is refreshingly free of unnecessary formal barriers and bureaucratic rituals that often complicate academic publishing without adding real value. The peer-review system is demanding yet constructive, guided by genuine scientific dialogue rather than hierarchical or authoritarian attitudes. Reviewers act as collaborators in improving the manuscript, not as gatekeepers imposing arbitrary standards. This journal offers a rare balance: high methodological standards combined with a respectful, transparent, and supportive editorial approach. In an era where publishing can feel more burdensome than research itself, this platform restores the original purpose of peer review — to refine ideas, not to obstruct them Prof. Perlat Kapisyzi, FCCP PULMONOLOGIST AND THORACIC IMAGING.
Dear Mercy Grace, Editorial Coordinator of Obstetrics Gynecology and Reproductive Sciences, We would like to express our gratitude for your help at all stages of publishing and editing the article. The editors of the magazine answer all the necessary questions and help at every stage. We will definitely continue to cooperate and publish other works in the Obstetrics Gynecology and Reproductive Sciences! Best wishes from, Alla Konstantinovna Politova,
